Reconstructive
Procedures for HIV-Related Lipoatrophy
(Updated
March 2008)
By Nelson Vergel, BsChE, MBA
Founder, Program for Wellness Restoration,
PoWeR, a 501( c ) 3 non profit educational organization
(http://www.powerusa.org)
Facial
wasting has become an important issue in the lives of those
living with HIV. HIV status sometimes becomes apparent just
by looking at someone’s face. Self-image and self-esteem
issues among People living with AIDS are further exacerbated
because of this daunting problem.
A poster presentation at the second International Workshop on
Adverse Drug Reactions and Lipodystrophy in HIV in Toronto September
12-15, 2000 that dealt with the issue of “erosion of self-image
and self-esteem, problems in social and threats to locus control,
anxiety around HIV disclosure forced by noticeable body change,
and a propensity to demoralization and depression” (Collins,
Abstract P36).
Some
living with HIV related lipodystrophy have minimized visceral
fat (“protease pouch”) accumulation with the use
of nutritional, exercise, anabolic therapies and insulin sensitizers
and by switching HIV medications. However, facial wasting and
the loss of subcutaneous fat under the skin of the buttocks
and extremities (arms and legs) are problems for which we have
found no systematic solutions to treat the problem at the causative
level.
Some
studies that have followed up patients after they switch from
protease inhibitors to non-nucleoside analogs have not found
statistically significant changes in body composition. A study
presented by Saint Marc, et al, and the Retrovirus Conference
in Feb 2000 found that the loss of subcutaneous fat could be
reversed partially by switching from Zerit (Stavudine or D4T)
to Abacavir (Ziagen) or Combivir combinations. Dr. Andrew Clark
from South Africa also presented a poster (Abstract P85) that
showed some improvement of facial wasting after switching from
Zerit to an alternative NRTI in 10 of 11 patients after 6 months.
However, after discussion, all concur, that though these studies
show some reversal of this problem, the fat gains in the face
are very slow in coming and not sufficient to restore the original
appearance of someone’s face. For more on Zerit and fat
loss visit:
http://www.medibolics.com/LipoatrophyandAntiretroviralDrugChanges.htm
and http://www.hivandhepatitis.com/hiv_and_aids/lipo/lipo8a.html.
Out of despair and necessity, many people living with HIV have
in the last decade have been seeking reconstructive options
to address wasting in their faces, buttocks and extremities.
For results of a survey of over 800 people to learn about the
main products and options used in the community, please visit:
Survey
Results
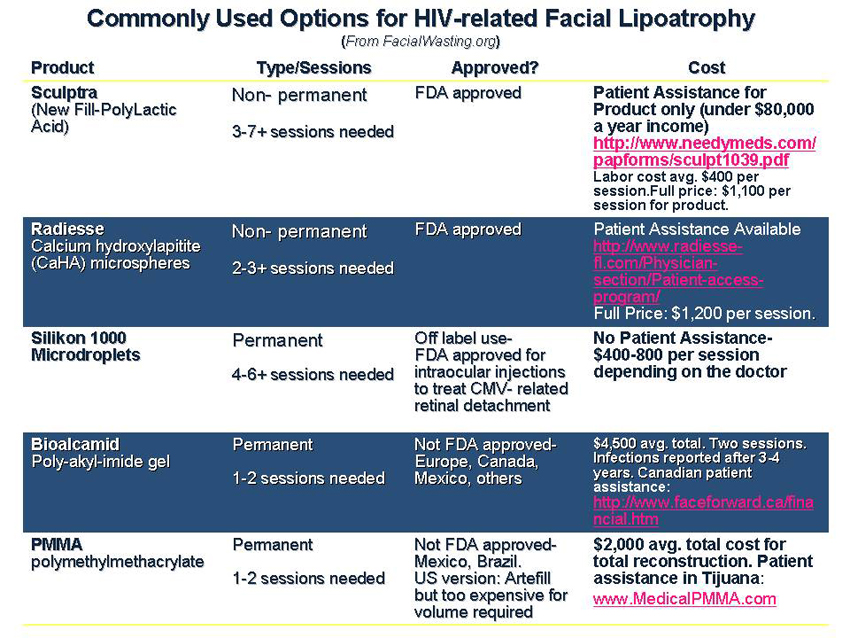
Cosmetic products including Collagen, Fascian,
Alloderm and silicone injections, along with more traditional
medically reconstructive agents such as L-polylactic acid (now
branded as Sculptra), polymethylmethacrylate (PMMA), and assorted
poly-acrylamide type gels (BioAlcamid), Silikon 1000 and Radiesse
are currently being sought out by many. The cost of these treatments
are often borne by patients who have had to cash-out life insurance
policies and sell property to pay for these costly procedures.
Such treatments are rarely covered by insurance companies who
often dismiss them as ‘cosmetic’ and not medically
necessary. While California now mandates that reconstructive
procedures be covered at least in part by insurance, the process
of reimbursement is difficult time consuming and not patient
friendly.
What
products and techniques are available? Who are the providers?
In
the last several years there has been a shakeout in the available
products and techniques of treatments for what we now call HIV
associated soft tissue wasting or lipoatrophy. Several techniques
previously popular such as antilogous fat grafting and micronized
injectible fascia tissue (Fascian), Teflon paste, surgical implantation
of Gore-Tex and ‘hard silicone’ solid implants have
fallen off the radar of HIV facial wasting reconstruction options,
while new products such as Sculptra, Arterfill (PMMA), Radiesse
have been approved for use by the FDA. Other “off-label”
product such as Silikon 1000 microdroplet injections are also
being used extensively.
The
products and how they are used
Where
are implants placed?
Skin is divided into layers, epidermis, dermis and hypodermis.
Underneath the skin is fat and muscle which is covered by fascia.
The epidermis mainly is composed of dead cells, while the dermis
contains extracellular matrix, nerves, vasculature, and other
structures.
Soft
tissue fillers are injected into different layers of the skin
and underneath it depending on their composition and properties.
Fillers such as Collagen, Restyline, Radiesse, Sculptra, some
PMMA compounds and microdroplets of liquid silicone oil are
injected into the dermal layer, which allows for incorporation
of the material by the skin.
Bio-Alcamid
is injected deep under the skin in the area previously occupied
by fat. Some PMMA products are injected deep under the fascia
and muscle while solid silicone implants are attached directly
to bone.
Key
Options for facial reconstruction
Hard Silicone Solid Implants
Some
plastic surgeons recommend solid cheek implants for treatment
of sunken cheeks. These hard solid silicone implants are very
popular and have been used extensively in the entertainment
industry. The good thing is that they are permanent, safe, and
give you lots of volume. Some people feel that the end result
is somewhat "feminine," and in people with HIV, a
real problem is that the loss of fat is so severe that the thinned
skin leaves the edges of the implant visible. In Los Angeles,
Dr. William Binder (http://www.doctorbinder.com/)
utilizes custom-designed implants using 3-dimensional computer
modeling that fit perfectly in the actual deformity. Another
doctor that has had good results with implants for facial lipoatrophy
is Dr. Stacey Silvers in New York City. You can find more information
about her work at http://www.nysinuscenter.com/
Sculptra
(polylactic acid, old name: NewFill)
The
following clip from Project inform is by far one of the best
histories and descriptions available and can be found in its
original at http://www.projinf.org/tan/advo102004.html
In August
2004, the FDA approved Sculptra (a poly-L lactic acid
formerly known as NewFill) for the restoration and/or
correction of the signs of facial fat loss due to HIV
related lipoatrophy (i.e. facial wasting). The company,
Dermik Aesthetics, filed for approval based on European
studies in 278 people with severe facial wasting. The
majority of those studied were white men aged 41–45
years, nearly all of who were on anti-HIV therapy. People
received three to six rounds of Sculptra treatment, consisting
of multiple small injections, at two-week intervals. Volunteers
were then monitored for two years. Roughly 40% of people
studied had a significant lasting increase in the volume
of tissue in their cheeks for up to two years following
the series of injections. Quality of life measures (i.e.
anxiety and depression surveys) also improved significantly.
This is key given facial wasting is linked with depression
and a reduced ability to adhere to anti-HIV regimens.
Sculptra causes
scar tissue (i.e. collagen) to collect in the areas where
it is injected. The amount of Sculptra injected and the
method and placement of each injection can strongly impact
the results. Proper training is essential to achieve the
best results. It can cause very small lumps called micro
nodules to form in up to 44% of people receiving it. The
micro nodules are not usually visible or the source of
ongoing inflammation and infection—as with other
types of injectible fillers—but they can often be
felt under the skin. Although most doctors use a numbing
agent like lidocane when injecting Sculptra, there is
usually mild to moderate pain during the injections. Sculptra
can also cause tenderness, swelling and bruising at the
site of injection. This typically goes away within days.The
level of fullness resulting from each round of injections
varies from person to person. People with more extreme
facial wasting will sometimes require more than six rounds
of injections to achieve lasting results. There are little
data on the long-term use of Sculptra, or on its use in
women and people with darker skin.
The FDA placed two conditions on Sculptra’s approval.
First, the company may not encourage its use for cosmetic
purposes in people not infected with HIV (e.g. to fill
in wrinkles). The company also agreed to conduct an open-label
study of 100 volunteers for five years to evaluate Sculptra’s
long-term safety. The study will include at least 30 females
and 30 people with dark skin types.
When Sculptra was owned, manufactured and distributed
by its inventor, Dr. Elisabeth Laglenne, it was typically
available for sale in Europe or Mexico for as little as
$200 per kit (two vials). Just prior to Sculptra’s
FDA approval, the buyer’s club DAAIR in New York
sold it for $400 per kit. Post approval, Sculptra is now
selling for about $960 per kit. Thus, Sculptra now costs
more than twice as much as it did before approval. Activists
have been told that its price will be increased in Europe
and elsewhere accordingly. In these countries it will
continue to be sold as New-Fill. |
While the cost Sculptra has risen
and there are also professional fees charged by the doctor for
injecting it. Thanks to the efforts of HIV advocates and willingness
from the manufacturer, Dermik- Aventis, a good patient assistance
program has been implemented that helps patients with incomes
under 80,000 dollars a year.
Note
on Dermik's patient assistance program:
The direct line to the Dermik Patient
Assistance Program: 866-310-7551.
Along with the application form
that they will fax or send you, which your doctor has to send
in to them once you've filled it out, you'll need to send them
your last year's tax returns - 1040. In order to receive Sculptra
free, your income cannot be above $40K - there is no low end
requirement. If it's below $40K you get up to six kits (each
kit contains two vials) for free - two kits at a time –
that Dermik sends it directly to your Doctor.
If your income falls in the $40
- $80K range, Dermik will sell you the kits on a sliding scale;
the patient is responsible for the doctor's fee for each treatment
which ranges from $350 up to $500, or more depending on who
you go to see.
Once you're approved for the program
by Dermik, the approval is good for 18 months, after which you'd
have to apply again.
Elsewhere on this site there is
a sample letter for submitting to 3rd party payers. For the
latest details of the Sculptra Patient Assistance Program and
to find doctors in your area, go to www.Sculptra.com.
You can also view the form here:
http://www.needymeds.com/papforms/sculpt1039.pdf
Dr
Doug Mest (DrMest@aol.com)
in Hermosa Beach, CA and Dr Gervias Frechette (GERVAISFRECHETTE@aol.com)
in NYC and San Francisco, are among the most experienced doctors
working with Sculptra and have trained many US doctors for Dermik.
You can find a doctor in your area by typing your zip code or
city in the box at the top right hand side of this page:
http://www.sculptra.com/us/
Comments
about Sculptra:
Sculptra has shown good results in those with mild
to moderate facial wasting. In those patients with more servere
cases, this options turns out to be too expensive even for those
helped by the patient assistance program. Mild to moderate cases
require from 3-5 sessions. More severe cases require over 8
sessions. Most doctors are charging 300-600 dollars per session
for injecting it. Many people get disappointed when results
start wearing off and they need yearly touch-ups. But some people
love it and are happy that it is not a permanent product that
may have long term consequences. To read and share experiences
with others subscribe to our discussion list by sending a blank
email to pozhealth-subscribe@yahoogroups.com
or look at the chat room in this site: http://facialwasting.org/chat.htm
Radiesse
(formerly Radiance)
Primarily
used in cosmetic and facial “rejuvenation”, Radiesse
is being used more often in HIV facial reconstruction because
of its FDA approval for HIV facial lipoatrophy (it is the only
approved agent for this indication besides Sculptra). Their
web site is http://www.radiesse-fl.com.
Radiesse is chemically, calcium hydroxylapitate, (CaHA). Microspheres
are suspended in an aqueous polysaccharide gel for the injectable
version for use as a skin filler. It is manufactured by Bioform
of Franksville, Wisconsin. It is not a permanent solution for
facial wasting and like Sculptra, touch ups are required after
a year to 18 months in most cases.
Calcium
hydroxylapitate has safely been used in the body for many applications
including dental applications where bone build-up is needed
for reconstruction and also in block form for cosmetic implants
such as cheek, jaw, cranial and chin implants (hard bony areas).
Calcium hydroxylapitate creates a lattice where the surrounding
cells can be incorporated from ossification in bony areas to
a stable scaffold in which soft tissue can grow. The calcium
hydroxylapitate microspheres are suspended in a polysaccharide
carrier which holds the microspheres in place until it is reabsorbed
and the collagen takes place. When injected in soft tissue,
away from bone, fibroblasts work by building reportedly a non-scar
tissue collagen type, creating volume in the treatment area.
Cost
to the practitioner is about $200 - $275 per 1.3 cc syringe.
So with labor and markup doctors are charging $500 to $1000.00
per syringe. For HIV facial lipoatrophy, depending on the severity,
it may take 10 to 20 syringes, so the might vary between $5000
and $20,000 to achieve a full correction.
However, Radiesse now has a patient assistance program( http://www.radiesse-fl.com/What-is-Radiesse/How-much-does-it-cost
) for people with HIV. For those with a yearly income under
$40,000, the program will provide 6 syringes (per year) at a
cost of $75 per syringe. This does not include the injection
fee and in most cases 6 syringes does not provide enough product
to achieve a full correction. It is possible to request extra
syringes, but the provider must submit additional documentation.
You can search a doctor here: http://www.radiesse.com/start/search.html
Silicone
Microdroplets (Silikon 1000 or SilkSkin)
Silicone
microdroplets, along with Arterfill (PMMA), is a permanent solution
to facial wasting. It is not FDA approved for facial lipoatrophy
but doctors use it legally in an “off-label” use
since it was originally approved for cytomegalovirus (CMV)-related
retinal detachment.
The following information is from Richard James Company, the
manufacturers of SilSkin brand of liquid silicone oil.
Microdropplet
liquid silicone injections build soft-tissue by encouraging
the production of new collagen, the skin's natural structural
protein. Silicone injections are used primarily to fill
depressions such as may be seen in HIV lipoatrophy.
Microdropplets of LIS are injected into the skin at multiple
points (the microdropplet serial-puncture technique) with
a slender, sterile needle. Because LIS is chemically inert,
it remains a liquid after injection and is not altered
or changed by the body. Over a period of months, microdropplets
of LIS stimulate skin cells (known as fibroblasts) to
produce new collagen around each microdropplet. Once a
microdropplet is surrounded, collagen production stops.
Through repeated injections over several months the combination
of LIS microdropplets and new collagen gradually fills
depressions. Slight swelling may be seen immediately after
injection, giving the appearance of instant improvement;
however, this swelling subsides in several days.
At the onset of treatment, visits are usually spaced at
one month intervals. Ordinarily, desired improvement is
not achieved until after several visits. The number of
treatments depends on the depth of the depression(s) or
the degree to which a facial contour is to be enhanced.
As the desired degree of soft tissue augmentation is approached,
visits are scheduled at three to six month intervals,
or longer. Because LIS and the collagen it stimulates
are long lasting, it is important to allow sufficient
time to elapse between treatments to observe the amount
of soft tissue formed and thus avoid over correction.
Furthermore, although LIS corrects previous loss of soft
tissue, it cannot prevent future loss caused by aging,
repetitive facial muscle action or progression of lipoatrophy.
Maintenance injections at six to twelve month intervals
may be desired to treat additional soft tissue loss as
time passes. |
SilSkin
remains only for testing in clinical trials, but a similar formulation
to SilSkin is Silikon1000 which is approved for use in the eye
for treating detached retinas attacked by a virus called CMV.
It is this product that is being used off label in microdroplets
as a skin filler.
These are the only medically approved formulations of silicone
oil and the manufacturers go to great lengths to differentiate
them form older, impure and industrial grades of silicone oil.
Additionally the manufacturers of SilSkin emphasis that silicone
oil should only be implanted with the microdroplet procedure,
where many hundreds if not thousands of micro drops are injected
to create volume rather than the wholesale injection of large
amounts at one time which would predispose the implant to migrate
with gravity.
The cost of microdroplets varies widely and can run up to $800
per visit ( the more compassionate doctors are charging $250-
$300) as the technique of applying hundreds or thousands of
microdroplets is highly labor intensive. Mild to moderate facial
wasting cases may require 4-6 sessions while more severe cases
may require up to 20 sessions. There is no patient assistance
program for this product. Several doctors around the county
are using it but we do cannot find a web site that lists them.
Dr Derek Jones in Los Angeles, Dr Brad Bowden in Houston, Dr
Orentreich in New York City, Dr Hal Brody in Atlanta, and Dr
Carruthers in Vancouver have used the product successfully for
years.
Dr. Derek Jones's web site is http://www.drdjones.com/519575.swf
and Dr Orentriech (New York City) web site is http://www.orentreich.com/
. Dr Carruthers’ web site is http://www.carruthers.net
and he is available for questions and consultations via email:
helen@carruthers.net
or phone: Toll Free: 1-877-714-8222. There is also
a doctor in Florida using the microdroplet technique:
Barry I. Resnik, MD. Resnik - Dermatology Aventura, FL (telephone
305-692-8998) www.resderm.com
Bio-Alcamid (poly-akylimide gel)
Manufactured in Italy, and widely available in Europe
and Mexico, Bio-Alcamid was approved in Canada in 2004 for treating
facial wasting. It is a permanent product with the fastest results
in the market. It is not approved by the FDA (as of March 2008)
but a U.S. company just acquired its rights and will proceed
with the required FDA paper work to get it approved in the US.
Other polyacrylamide hydrogels (known as Aquamid) have been
available in various preparations for 3 decades in different
countries. Used mainly in Eastern Europe and Russia, there gels
had several well
documented complications including infection, migration,
and release of toxic acrylamide monomers. All of these complications
become aggravated over time. For more information , read this article Bio-Alcamid Blues and this paper Late-Appearing Abscesses.
Some 7 years ago, Polymekon, the Italian company that manufacturers
Bio-Alcamid, bought the rights to an existing acrylamide gel
and reformulated it with the claims that the new product, Bio-Alcamid,
did not release toxic acrylamide monomers, did not degrade and
did not migrate. They claim that their product was not a polyacrylamide
but a poly-akylamide. We are yet to find someone who can explain
what the difference is between those two molecules.
The seeming safety and permanence of this product made many
patients rush to Tijuana, Mexico to get a permanent solution.
Bio-Alcamid has been widely used in Italy, the UK, Mexico and
Canada since 2002. Best known for the use of the product was
the Mexican Clinic’Estetica during the time it was led
Anna Love and by Dr. Luis Casavantes as medical director.
BioAlcamid was approved in Canada in April 2006. You can visit
this site for more details: http://www.faceforward.ca/
This is a report from a patient who got BioAlcamid in Canada.
Look also at the links he provides at the bottom of the article:
http://www.positivelypositive.ca/articles/lipoatrophy.html
It became apparent after a few years from reports coming from
medical practices around the world including from Italy where
the product was developed, that many physicians and patients
were reporting higher than expected complication rates, mainly
infections.
In the interview of Dr. Casavantes, who has performed more Bio-Alcamid
implants than any other doctor, expressed his view that the
high complication rate for these implants, perhaps 7% to 10%,
stem from 2 main causes: a not-fully sterile field on the skin
surface and the concomitant capture and injection, at the time
of the procedure, of pathogenic skin bacteria (staphylococcus
aureus, micrococcus luteus, staphylococcus epidermis and methicilin
resistant staph aureus) and poor placement of the implant by
not well trained practitioners.
Dr. Garza (http://www.everardogarza.com)
used to charge $80.00 per ml. But recently the manufacturers
have pulled the product from the Mexican market. Dr. Garza is
now employing other fillers including PMMA.
We caution patients about potential long term complications
with this product. It forms a “pocket” of material
that can become a perfect medium for bacteria growth if punctured.
Polymethylmethacrylate (PMMA)
PMMA has been used for many years in reconstructive
medicine as a bone bonding agent because of its unique ability
to form a lattice structure which encourages infiltration by
osteoblasts (cells
that arise
from fibroblasts
and which, as they mature,
are associated
with the production
of bone)
if placed in bone. In skin, PMMA also promotes fibroblast and
vascular infiltration of the soft tissues it is implanted in
leading to a high safety profile vis-a-vis non-vascular implants
such as acrylamide gels and silicone oil. Most of the volume
gained from PMMA filler is the body’s own tissues and
blood vessels growing into the PMMA. And as the PMMA matrix
does not dissolve like Radiesse (calcium hydroxylapitate or
Sculptra L-polylactic acid, the implant is considered permanent.
PMMA is available in the United States under the trade name
of Artefill (http://www.artefill.com/consumer/).
This formulation was developed and approved after many years
of clinical trials by Dr. Gottfried Lamperle, but for one indication
only; filling the deep folds next to the nose called the nasio-labial
fold. Unlike Sculptra and Radiesse, this product is not FDA
approved for HIV-related facial lipoatrophy. The single reported
complication appearing in clinical trial results of ArteFill®
and its predecessor products have been a small number of tiny
palpable granulomas. The clinical experience suggests that granulomas
with PMMA tend to develop in thin skin areas or when the product
is dermally injected in a too shallow fashion. These granulomas
often respond to treatment with Kenalog 40, a powerful glucocorticod.
As ArteFill® was developed and purified over several generations
from the original Atreplast, the appearance of granulomas have
decreased dramatically. We also have noted from the clinical
experience that NewPlastic® does not seem to produce granuloma
formation when grafted sub-facially in the Nacul/Casavantes
technique discussed in detail below.
ArteFill® costs medical providers $2,100.00 per 1.2 ml prepackaged
in a box of 2 syringes containing 0.8 and 0.4 ml of product.
This kit and the professional services of the provider are often
sold to the patient for $3,500 to $4,000, thus making it impractical,
as a corrective for large volume tissue loss. At a cost to the
patient of $3,500 for the treatment, the per ml price comes
to $2,917. Common in the faces of people with HIV tissue loss,
are deficits which can require from 30 ml to 40 ml of filler.
A face requiring 30 to 40 ml of Arte-Fill® would cost from
$87,510 to $116,680. This calculation leaves aside the issue
of the labor involved in administering the contents of 35 kits
with 70 small syringes necessary for such a procedure.
The only reported problem with PMMA in the trials was the development
of granulomas in thin skin areas; a concern of some significance
to HIV positive men and especially women suffering with the
depletion of fat in the skin. Many patients are attracted to
PMMA because of its permanence and lack of ‘touch-ups’
necessary with the temporary or long lasting implants. Some
patients also report small bumps that may be smoothed out by
follow-up work.
Brazilian esthetic medicine doctors and dermatologists have
been using PMMA as a treatment for HIV associated soft tissue
wasting for the better part of a decade, virtually from the
start of the identification of lipodystrophy syndrome.
Dr. Márcio Serra (http://www.clinicamarcioserra.com.br)
has been in practice for almost two decades and has become well
known as a major provider of PMMA soft tissue augmentation and
reconstruction threrapies in Brazil. Dr. Serra has treated a
great many HIV positive patients and had worked with HIV skin
pathologies virtually from the start of the epidemic. Dr. Serra
is a consultant to the Brazilian government on HIV lipoatrophy
and has trained dermatologists and plastic surgeons treating
HIV lipoatrophy throughout Brazil.
Dr. Serra began using a compounded PMMA in the trials he ran
for the Brazilian government, treating HIV positive patients
needing facial wasting corrections almost 10 years ago.
Perhaps the most remarkable work Dr. Serra has done was the
study culminating in a law providing free facial wasting treatments
for patients in public hospitals. Your author can’t help
but cringe at the thought of how difficult and expensive it
is to get any treatment for HIV lipoatrophy in the United States,
while in Brazil, thanks to Dr. Serra, medical care of this sort
is given freely to those who need it.
Since September/October of 2007, ANVISA, the Brazilian health
authority has outlawed the compounding of PMMA products. Since
that time, there have been only two legally available PMMA products
in Brazil, Metacrill® and NewPlastic® and since then
Dr. Serra has switched over to Metacrill® which he has informed
us is double the price of the older compounded product he had
used. He accounts his price increases to this issue as well
as the weakness of the US dollar.
From the photographs on his web site and from reports from patients,
Dr Serra apparently uses a cross thatching technique with subcutaneous
injections only utilizing conventional needles.
We were unable to trace any reported complications or adverse
reactions from Dr. Serra’s approach or PMMA products.
However the clinical and preclinical research of Dr. Gottfried
Lemperle, an expert on PMMA formulations and professor at the
Universityof California in San Diego, suggests that there are
greater incidents of palpable nodules and granulomas when PMMA
is injected too superficially. One correspondent, a physician
from Miami has reported minor and non-troublesome granulomas
as a result of treatment with the subcutaneous approach. In
general, people on pozhealth@yahoogroups.com
who have traveled to Rio de Janeiro to use his services are
generally pleased with the results.
NewPlastic®, was developed in Porto Alegra, Brazil by Dr.
Almir M. Nacul. Dr.
Nacul is in clinical practice and is recognized as the inventor
of Bioplasty (soft tissue augmentation with fillers) and has
authored a medical textbook and many
articles on soft tissue augmentation with PMMA. NewPlastic
is the commercial name for a series of PMMA, products with microspheres
of 40 to 60 microns, in different concentrations. These products
are currently available as 2%, 10% and 30% concentrations of
PMMA in a vehicle of 98% 90% and 70% methylcellulose, respectively.
Dr. Nacul is also developing a 40-45% concentration for specific
reconstructive applications where a denser implant is desired.
NewPlastic® is approved and registered throughout South
America and in Mexico in North America.
Dr. Nacul’s practice is more expensive then Dr. Serra’s
and does not focus on HIV. He has made his reputation for developing
the “Brazilian Butt Lift Bioplasty” technique for
butt enhancement with PMMA delivered via micro-canula and a
specially engineered hand piece which meters out PMMA very precisely.
Dr Nacul is closely collaborating with Dr. Luis Casavantes of
Tijuana, Mexico (www.drcasavantes.com)
in bringing his micro-canula technique to North America.
Dr. Casavantes practice is primarily an HIV facial wasting treatment
clinic and dermatologic pathology practice. Dr. Casavantes uses
a number of technologies adapted and expanded from the work
of Dr. Almir Nacul’s Bioplasty. Employing rounded microcanulas
to replace conventional sharp needles with a metered implantation
device. The “PMMA Grafting Technique” (PGT) is touted
as “a breakthrough in patient comfort and reduced trauma”.
PGT avoids sharp needles and the damage they can cause when
used in areas dense with nerves and blood vessels as the face.
The round tipped microcanula easily travels under the skin and
fascia with little resistance and cannot damage vascular and
nerve bundle structures as needles do.
PGT uses only 2 to 3 entry points per side as opposed to the
50 or more injections used with conventional needle techniques
with accompanying reductions in trauma and bleeding and virtually
zero bruising. Plavix and other blood thinners are not contraindicated
by PTG.
Dr. Casavantes as of this writing charges $140.00 per ml for
facial reconstruction. Patients need to add the cost of air
fare to San Diego, meals and taxis to the clinic. We estimate
these ancillary costs come to $ 80.00 in addition to treatment
fees. Treatment with the Casavantes PGT usually takes 2 to 3
sessions. For patients on a limited income, Dr Casavantes offers
a patient assistance program with significantly reduced costs.
Click on the assistance tab on Dr. Casavantes’ medical
information site: www.MedicalPMMA.com
.
Dr. Casavantes has posted a video
of the microcanula procedure on line.
Reimbursement Issues
A few
insurers and HMO systems in the US are starting to pay for Sculptra
and/pr Radiesse (Kaiser Permanente in No CA and others). If
you need to negotiate with your insurance company to get them
to pay for product and/or labor , you may want to use this letter:
************************************************
Insurance
Co Name
Insurance
Co Address
Patient
Name
Subscriber
#
Date
To
Whom It May Concern:
This
letter is written in regards to the medical necessity of restorative
treatment for the facial deformities this patient suffers from
secondary to HIV-Associated Lipoatrophy. Facial fat loss is
the most devastating aspect of this condition as it can not
be disguised by clothing or other means. Although the exact
underlying mechanism of HIV-Associated Lipoatrophy is unknown
(1), the devastating effects of this condition are known (2,3).
Patients suffering from this condition are at an increased risk
of depression, socially withdrawn and potentially suicidal.
Furthermore, patients have even stopped their life saving HAART
therapy without consultation with their physician in an attempt
to stop this side effect. The implications for viral mutations,
increasing viral load and worsening of patients underlying condition
requiring more expensive treatments cannot be stressed enough.
Treatment of HIV-Associated Lipoatrophy with Sculptra (Poly-L-Lactic
Acid) has been shown to improve anxiety and depression scores
(4) as well as improve patient’s quality of life as measured
by visual analogue scale (5). The use of Sculptra is clearly
indicated as a reconstructive procedure; that is, repair of
abnormal facial structure caused by HIV or its treatment, in
order to create a normal appearance.
The safety and efficacy of Sculptra in restoring the normal
facial contours of patients suffering from HIV-Associated Facial
Lipoatrophy has been evaluated by the US FDA (6). Based on the
available scientific evidence (4,5), the FDA granted approval
of Sculptra as a restorative medical device for the specific
indication of HIV-Associated Facial Lipoatrophy in August 2004.
For your information. the ICD9 diagnosis code for lipodystrophy
is 272.6. HIV-related lipodystrophy syndrome consists of lipo-hypertrophy
(fat accumulation in the visceral area and dorsocervical pad)
and lipoatrophy (subcutaneous fat loss in the face, extremities
and buttocks).
Due to the medical necessity of this treatment and the availability
of a safe and effective treatment option, pre-approval is hereby
requested for treatment of this patient's HIV-Associated Facial
Lipoatrophy with Sculptra.
As this approval is relatively recent, I would be happy to further
educate your company on this issue in any way that you might
deem helpful. Please feel free to contact me at the above office
with any questions you may have.
Sincerely,
References:
1)
Montessori, V. CMAJ. 2004;170:229-238.
2)
James J, Carruthers, A. Dermatol Surg. 2002;28:979-986.
3)
Martinez, E. Drug Saf. 2001;24:157-166.
4)
Moyle, GJ. HIV Medicine. 2004;5:82-87.
5)
Valantin, M. AIDS. 2003;17:2471-2477.
6)
FDA Scientific Advisory Panel 3/25/2004 Washington DC
Conclusion
The
impact of facial lipoatrophy on self-image and self-esteem has
been devastating for the entire community of people living with
HIV.
Some treatments for HIV related soft tissue wasting have emerged.
Patients now have access to various products and services in
the US but many more permanent and cost effective options are
available in Canada, Mexico, Europe and Brazil.
Some options may require frequent touch ups, some are long term
and others are permanent.
In all instances, including US approved treatments; the patient
has to pay amounts that range from two thousand to eight thousand
dollars while at the same time little to no reimbursement is
currently available for some of these treatments.
There are limited long-term HIV specific data available, so
it is difficult to assess long term safety. Current information
is limited to small studies with no clinical data other than
before and after pictures.
A comprehensive and effective advocacy campaign is needed from
the HIV community to stress all important issues at the FDA
level for safe protocols and access to those who may want to
make an informed decision based on risks and benefits. Additional
advocacy in the area of reimbursement is also needed since these
are corrective measures that treat a drug induced side effect,
and like any other side effect corrective measures available,
it should be reimbursed by third party payers. Hopefully, we
will see a lot of activity on this issue in the near future.
For up-to-date information, join our free lipodystrophy discussion
group by sending an email to pozhealth at
pozhealth-subscribe@yahoogroups.com
A
great article to read besides the information provided below
is :
http://www.aidsmeds.com/lessons/Lipoatrophy1.htm
For
a list of providers and results of our lipodystrophy survey,
visit our next page: http://facialwasting.org/surveys_lists.htm
Other
resources to read:
http://www.hivandhepatitis.com/2004icr/aids2004/dos/0711/071104_f.html
http://www.prn.org/prn_nb_cntnt/vol9/num4/horn_v9n4_frm.htm
http://www.aidsmeds.com/lessons/Lipoatrophy9.htm
http://www.i-base.info/htb/v6/htb6-1/Restorative.html
Address comments or concerns to Nelson Vergel at powertx@aol.com



